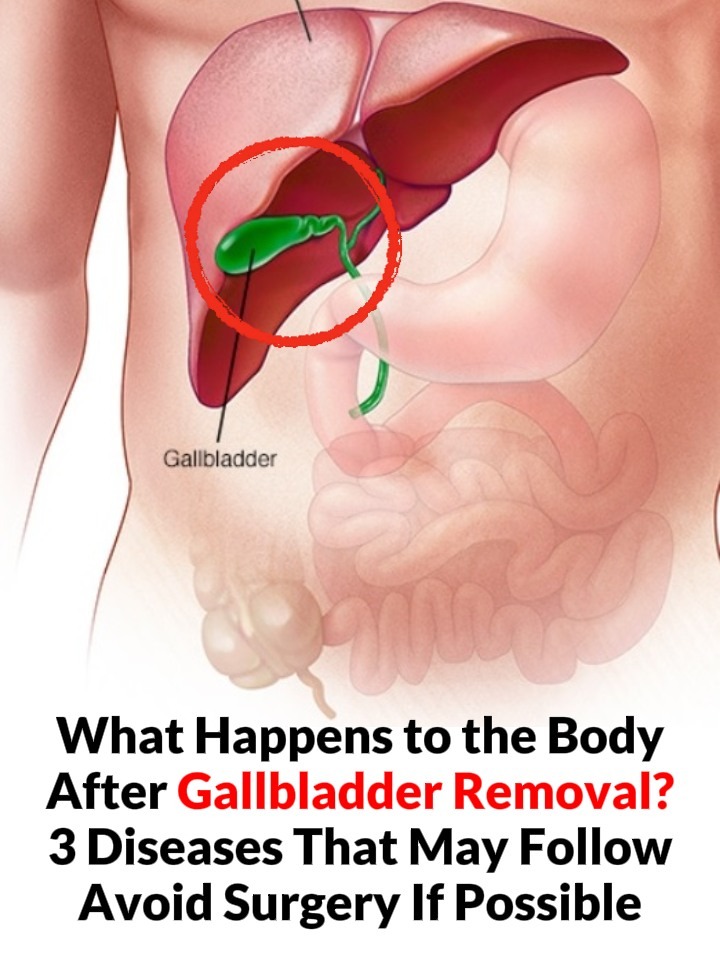
What Happens to the Body After Gallbladder Removal?
3 Diseases That May Follow – Avoid Surgery If Possible
Gallbladder removal, medically known as cholecystectomy, is one of the most common surgeries worldwide. Doctors often recommend it for gallstones, inflammation, or gallbladder dysfunction. While the operation is generally considered safe and lifesaving in certain cases, many people are unaware that living without a gallbladder can lead to long-term changes in digestion and metabolism. For some individuals, these changes may increase the risk of certain health problems.
Understanding what happens to the body after gallbladder removal can help you make informed decisions and explore alternatives when surgery is not absolutely necessary.
What Is the Gallbladder’s Role?
The gallbladder is a small, pear-shaped organ located beneath the liver. Its main job is to store and concentrate bile, a digestive fluid produced by the liver. Bile helps break down fats and absorb fat-soluble vitamins such as A, D, E, and K.
When you eat a fatty meal, the gallbladder releases bile into the small intestine in a controlled way. This timing and concentration are important for efficient digestion.
After gallbladder removal, bile no longer has a storage reservoir. Instead, it flows continuously and less concentrated from the liver directly into the intestine. While the body can adapt, this change may create digestive and metabolic challenges over time.
What Changes After Gallbladder Removal?
In the short term, many people experience:
- Diarrhea or loose stools
- Bloating and gas
- Fat intolerance
- Abdominal discomfort after meals
For some, these symptoms fade within weeks or months. For others, they persist and may evolve into chronic conditions.
1. Bile Acid Diarrhea (Chronic Digestive Disorder)
One of the most common long-term issues after gallbladder removal is bile acid malabsorption, often called bile acid diarrhea.
Why it happens:
Without the gallbladder regulating bile release, excess bile can spill into the colon. Bile acids are irritating to the intestinal lining and can pull water into the bowel, leading to frequent, urgent diarrhea.
Common symptoms:
- Chronic watery diarrhea
- Urgency after meals
- Abdominal cramping
- Burning sensation in the rectum
This condition is often misdiagnosed as irritable bowel syndrome (IBS), leaving patients untreated for years.
2. Fatty Liver Disease (Non-Alcoholic Fatty Liver Disease – NAFLD)
After gallbladder removal, the liver must work harder to continuously produce bile. Over time, this constant demand can disrupt fat metabolism and insulin sensitivity.
How it may develop:
- Continuous bile flow alters fat digestion
- Increased fat accumulation in the liver
- Higher risk of insulin resistance
This can contribute to non-alcoholic fatty liver disease, a condition where excess fat builds up in liver cells.
Warning signs:
- Fatigue
- Right-sided abdominal discomfort
- Elevated liver enzymes
- Often no symptoms in early stages
If left unmanaged, fatty liver disease can progress to inflammation, fibrosis, and even cirrhosis.
3. Increased Risk of Metabolic Disorders
Research suggests that gallbladder removal may be associated with a higher risk of metabolic syndrome, which includes:
- Type 2 diabetes
- High cholesterol
- Obesity
- Cardiovascular disease
Why the risk increases:
The gallbladder plays a role in bile signaling, which affects glucose metabolism and gut hormones. Removing it may disrupt these signals, contributing to blood sugar instability and weight gain in some individuals.
People who already have insulin resistance, obesity, or poor dietary habits may be more vulnerable to these effects.
Nutrient Deficiencies After Gallbladder Removal
Because bile is less concentrated, fat digestion may be less efficient. Over time, this can lead to deficiencies in:
- Vitamin A (vision and immunity)
- Vitamin D (bone health and immunity)
- Vitamin E (antioxidant protection)
- Vitamin K (blood clotting)
Symptoms may include weak bones, poor immunity, dry skin, and fatigue.
Can Gallbladder Surgery Be Avoided?
In some cases, yes—especially when gallstones are small, symptoms are mild, or inflammation is not severe.
Non-surgical approaches may include:
- Dietary changes (low-fat, whole foods diet)
- Weight management
- Adequate hydration
- Managing insulin resistance
- Certain medications to dissolve cholesterol gallstones (in select cases)
However, surgery is necessary and lifesaving in situations such as:
- Severe or recurrent gallbladder attacks
- Acute cholecystitis
- Gallbladder infection
- Pancreatitis caused by gallstones
- Suspicion of gallbladder cancer
Avoiding surgery should never mean ignoring serious symptoms.
Living Well Without a Gallbladder
If gallbladder removal is unavoidable, many people live healthy lives with proper care:
- Eat smaller, more frequent meals
- Reduce greasy and fried foods
- Increase soluble fiber intake
- Monitor liver health regularly
- Supplement fat-soluble vitamins if needed (under medical guidance)
Final Thoughts
Gallbladder removal can be essential, but it is not a “minor” change for the body. The gallbladder plays a subtle yet important role in digestion and metabolism. For some people, its removal may increase the risk of chronic digestive problems, fatty liver disease, and metabolic disorders.
If surgery is suggested, it’s wise to discuss all options, understand potential long-term effects, and make lifestyle changes that support digestive and liver health. When possible and medically safe, prevention and conservative treatment may help you avoid surgery—and its lifelong consequences.